Dark spots can seem to appear overnight—lingering after breakouts, increasing after sun exposure, or developing during hormonal changes. If you’ve been wondering why your skin forms these uneven patches, you’re not alone. This guide breaks down the science behind the causes of hyperpigmentation, explaining how and why excess melanin is triggered in the skin. Backed by current skincare research and dermatological insights, we’ll clarify the key factors responsible—from UV damage to internal shifts—so you can better understand what’s happening beneath the surface and feel more confident managing and preventing future discoloration.
Sun Exposure: The Primary Driver of Uneven Skin Tone
First and foremost, ultraviolet (UV) radiation is the leading external cause of uneven skin tone. When your skin detects UV rays, specialized cells called melanocytes jump into action. Melanocytes produce melanin, the pigment that gives skin its color and acts like a built-in umbrella, absorbing and scattering harmful rays (think of it as your skin’s natural SPF—just not a high enough one). According to the Skin Cancer Foundation, daily UV exposure significantly accelerates pigmentation changes and photoaging.
Over time, this defense mechanism leads to visible marks. Freckles form after repeated sun exposure, especially in lighter skin tones. Solar lentigines—commonly called age or liver spots—develop when melanin clusters in concentrated patches. Unlike freckles, these don’t fade easily.
More importantly, sun-induced pigmentation is cumulative. In other words, five minutes of unprotected sun today can surface as dark spots years later. That’s why dermatologists consistently rank UV exposure among the top causes of hyperpigmentation in the section once exactly as it is given.
So what can you do? Apply a broad-spectrum SPF 30+ sunscreen every morning—even on cloudy days. Reapply every two hours outdoors. Pro tip: Use two finger-lengths of product for full face coverage. For deeper hydration support, explore the science behind hyaluronic acid and skin hydration.
The Aftermath of Inflammation: Why Blemishes Leave Their Mark

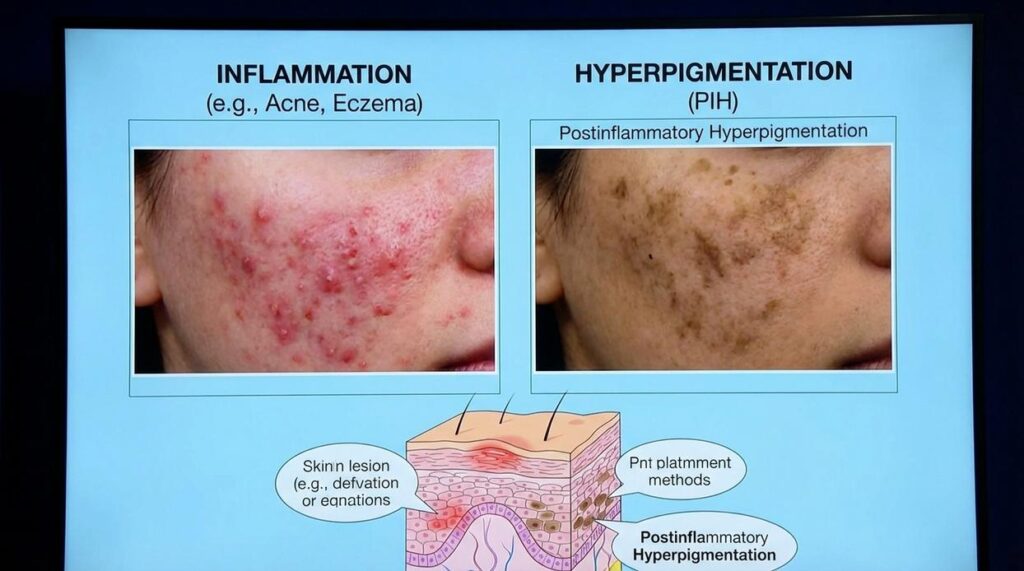
Post-Inflammatory Hyperpigmentation (PIH) is the technical name for those stubborn dark spots that linger long after a breakout or rash has healed. In simple terms, it’s discoloration that appears after the skin experiences trauma or inflammation. The injury fades. The mark doesn’t. (Annoying, right?)
Most people blame “bad skin” when they see these spots. I disagree. PIH isn’t about poor skin quality; it’s about an overenthusiastic healing response. When your skin is inflamed, melanocytes—the cells responsible for producing melanin, or pigment—kick into high gear. Sometimes they deposit excess pigment in the affected area, leaving behind a shadow long after the original issue is gone.
Common triggers include acne, eczema, psoriasis, bug bites, cuts, or even harsh scrubbing. Notice how many of these are everyday occurrences. This isn’t rare. It’s routine.
Here’s the twist: deeper skin tones are often more prone to intense and persistent PIH. That’s not a flaw—it’s biology. More active melanocytes mean more pigment production when inflammation strikes. Research published in the Journal of Clinical and Aesthetic Dermatology notes that higher baseline melanin increases the risk of visible discoloration after injury.
Prevention matters more than most people admit:
- Avoid picking or squeezing pimples
- Treat inflammation early
- Skip aggressive exfoliation during breakouts
Contrary to popular advice, scrubbing harder won’t fade marks faster. It often makes them worse. Sometimes the best skincare move is restraint (yes, even when the mirror tempts you).
Hormonal Shifts and Their Effect on Skin Pigment
Melasma is a type of hyperpigmentation marked by symmetrical, blotchy brown or gray-brown patches, most commonly on the cheeks, forehead, and upper lip. Because it often appears evenly on both sides of the face, it can look almost like a shadow laid across the skin (which is why some call it a “mask”).
So, what triggers it? In many cases, hormones. Fluctuations in estrogen and progesterone stimulate melanocytes—the cells that produce pigment—to make more melanin than usual. This is why melasma frequently develops during pregnancy (often nicknamed “the mask of pregnancy”), while taking birth control pills, or during hormone replacement therapy. In other words, the trigger is internal, not surface-level.
However, hormones alone don’t tell the whole story. Sun exposure acts as an amplifier, darkening existing patches and making them harder to fade. Even brief daily exposure can intensify discoloration. That’s why broad-spectrum SPF is non-negotiable (yes, even on cloudy days).
Unlike post-inflammatory hyperpigmentation, melasma isn’t caused by a direct injury to the skin but by a systemic trigger. If you’re comparing different causes of hyperpigmentation, this distinction matters. For practical next steps, see this hyperpigmentation guide.
Lesser-Known Causes of Skin Discoloration
When people think about the causes of hyperpigmentation in the section once exactly as it is given they often blame sun exposure alone. But several lesser-known triggers deserve attention.
Medications and Treatments: Certain antibiotics (like minocycline), non-steroidal anti-inflammatory drugs (NSAIDs), antimalarials, and even chemotherapy drugs can stimulate excess melanin production or deposit pigment in the skin (American Academy of Dermatology). If you’ve noticed dark patches after starting a new prescription, this may be worth discussing with your doctor.
Certain Skincare Ingredients: Phototoxic reactions happen when ingredients such as lime extract or bergamot oil react with sunlight, leaving streaky dark marks. A classic real-world example? Lime juice on skin at the beach leading to “margarita burn.”
Medical Conditions: Addison’s disease can cause generalized darkening due to increased adrenocorticotropic hormone levels (NIH).
Genetic Predisposition: Some people are simply more prone to pigment changes.
Pro tip: Always patch-test new products before full application.
Your First Step Towards a Clearer Complexion
Hyperpigmentation doesn’t appear without reason. It’s most often triggered by UV exposure, inflammation, and hormonal signals—three powerful forces that stimulate excess melanin production and leave behind stubborn dark spots. Now that you understand these root causes, you’re no longer guessing at solutions. You can choose targeted skincare, commit to daily sun protection, and seek professional treatments that address your specific trigger.
This knowledge is more than information—it’s control. Instead of reacting to discoloration, you can prevent it. Take charge of your routine, protect your glow, and make every skincare decision with clarity and confidence.